Cases of monkeypox have been identified in travelers from countries where the disease is considered an endemic. As a result, the Centers for Disease Control and Prevention (CDC) has issued a Health Advisory in the United States.
As of June 3rd, 21 cases in the U.S. have been confirmed or suspected, including one case in Pennsylvania. As per the State Department of Health, there is a possibility the disease may spread. Monkeypox symptoms involve a characteristic rash, preceded by a fever, swelling of the lymph nodes, and other non-specific symptoms such as malaise, headache, and muscle aches. In the most recent reported cases, symptoms included lesions in the genital and anal regions. Note that the disease may be confused with more commonly seen infections like syphilis, chancroid, and herpes. The average incubation period for symptom to develop is 5 to 21 days.
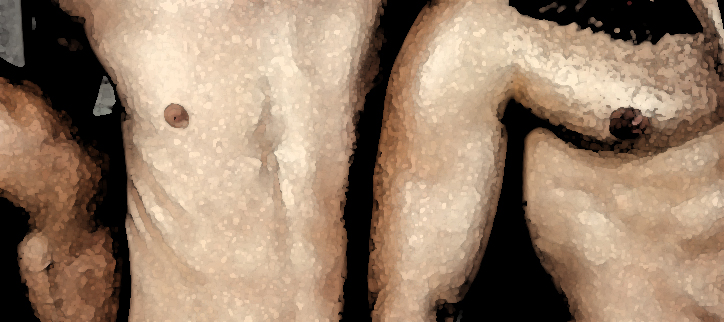
Monkeypox symptoms involve a characteristic rash, preceded by a fever, swelling of the lymph nodes, and other non-specific symptoms such as malaise, headache, and muscle aches. In the most recent reported cases, symptoms included lesions in the genital and anal regions. Note that the disease may be confused with more commonly seen infections like syphilis, chancroid, and herpes. The average incubation period for symptom to develop is 5 to 21 days.
Human-to-human transmission occurs through large respiratory droplets and by bodily fluids (like saliva and semen that can be transmission during sex) or coming in direct contact with a lesion. Respiratory droplets generally cannot travel more than a few feet, so prolonged face-to-face contact (like kissing) is more likely to spread the disease.
There is no specific treatment for monkeypox virus infection. However, the CDC reports that antivirals used to treat smallpox may prove beneficial. Monkeypox is generally mild and patients recover in a few weeks. The mortality rate is less than 1 percent in developed countries. There have been no deaths related to the monkeypox cases in the US so far.
There are FDA approved vaccines available to prevent monkeypox but these are not commercially available but are being made available to close contacts of known cases.
If you think you may be infected, contact your doctor’s office or local hospital first, for instructions. Going into your doctor’s office, or an emergency room, risks spreading the disease.
For more information about monkeypox, you can go to the CDC’s Health Advisory page. (https://wwwnc.cdc.gov/travel/notices/alert/monkeypox)







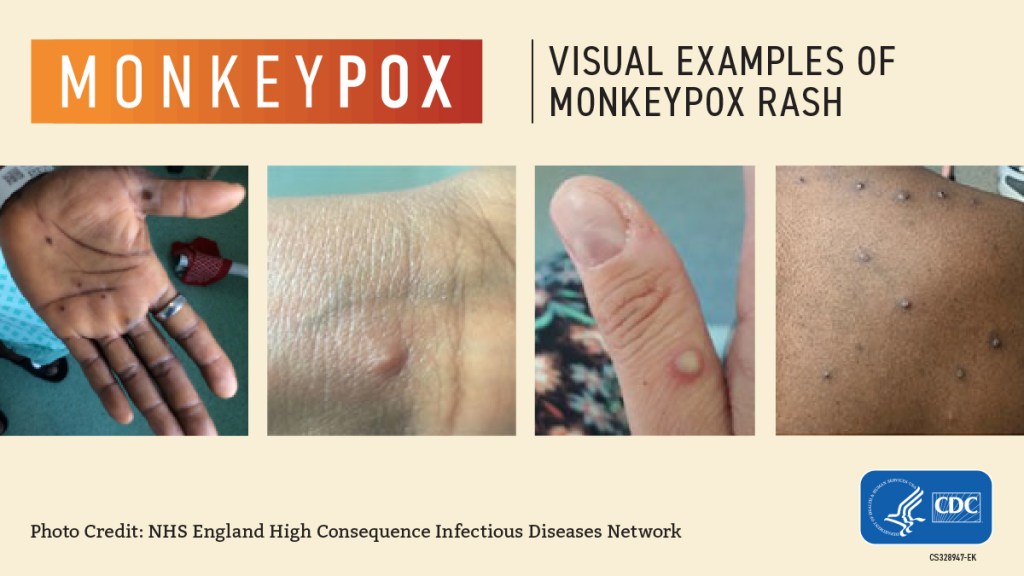
 Monkeypox symptoms involve a characteristic rash, preceded by a fever, swelling of the lymph nodes, and other non-specific symptoms such as malaise, headache, and muscle aches. In the most recent reported cases, symptoms included lesions in the genital and anal regions. Note that the disease may be confused with more commonly seen infections like syphilis, chancroid, and herpes. The average incubation period for symptom to develop is 5 to 21 days.
Monkeypox symptoms involve a characteristic rash, preceded by a fever, swelling of the lymph nodes, and other non-specific symptoms such as malaise, headache, and muscle aches. In the most recent reported cases, symptoms included lesions in the genital and anal regions. Note that the disease may be confused with more commonly seen infections like syphilis, chancroid, and herpes. The average incubation period for symptom to develop is 5 to 21 days.